Allergies. How do they influence outcomes in people with shoulder pain?
Article review of Patel et al., (2023)
Paper title and link to paper:
The effect of allergies on outcomes following shoulder arthroplasty: A national database analysis of 154,478 patients (Patel et al., 2023)
Overview of the paper:
In my current practice, I gain information on a patient’s allergies via their medical questionnaire and subjective assessment. In all honesty, when reviewing allergy information, I predominantly look for allergies that I may personally expose to a patient such as an allergy to latex or plasters. An allergy to medication or to food products may not be something I would consider that could have influence on outcomes.
The study we are looking at today was just released in Shoulder and Elbow by Patel et al., (2023). The authors completed a retrospective study using a US database from 2010 to 2021. They looked at patients with glenohumeral osteoarthritis who had a total shoulder arthroplasty. They split the patients into two groups. Those with allergies, and those without. This included any allergy, ranging from food to antibiotics and medication. The authors then reviewed post-operative complications. This was over 5 different time points for arthroplasty revision and for 30 and 90 days for other medical complications.
Odds ratio (OR)
Before reviewing the results, you may be want to recap on the statistical analysis the authors used. As well as looked at the p value for statistical significance, they also looked at the odds ratio (OR). This video gives you a good overview of OR but in summary:
OR < 1 - Exposure associated with lower odds of outcome
OR = 1 - Exposure does not affect odds of outcome
OR > 1 - Exposure associated with higher odds of outcome
Results
Revisions
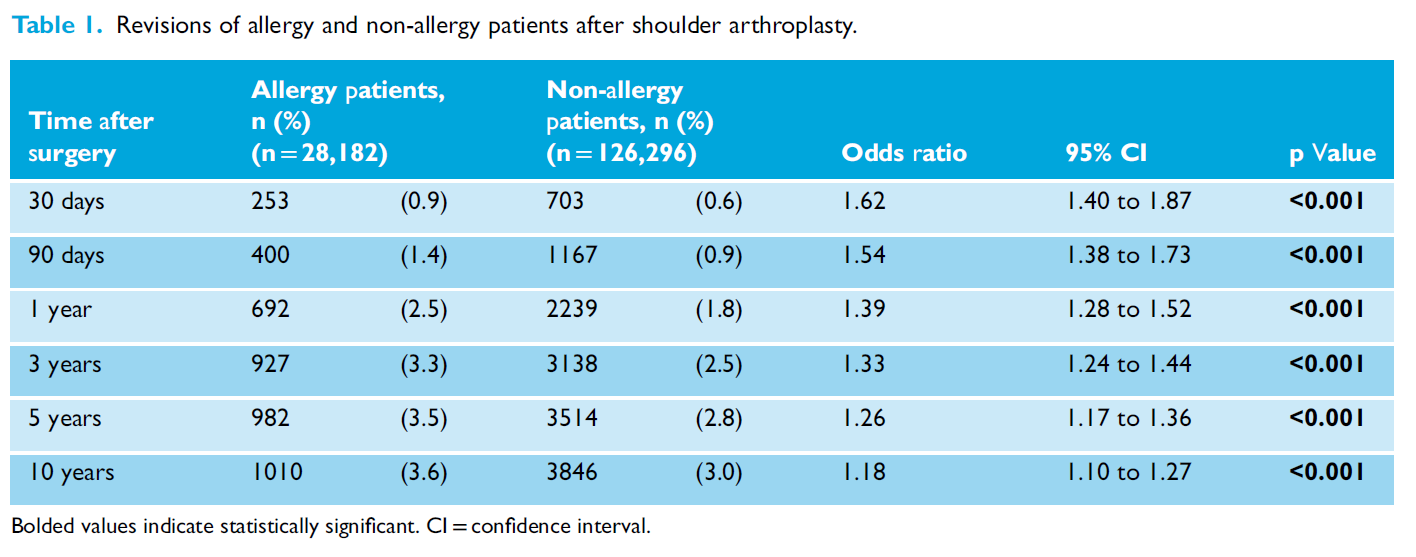
Patients with allergies were statistically significantly more likely to have a revision at all time points (see table 1 below). The OR at all time points were all greater than 1, with all the 95% confidence intervals not crossing over 1. This suggests we can be more confident of the OR findings.
Wound complications, joint infections, implant complications, and diagnostic complications
Table 3 looks at a further 5 different complication categories. As this study is based on looking at diagnostic codes for complications, we will get some overlap with some complication types. Implant complications refers to hardware loosening or breaking. Diagnostic complications refers to wound complications, post-operative stiffness, and prosthetic joint infection.
All of these categories suggest worse outcomes of those patients with allergies. Again, the OR at all time points were all greater than 1, with all the 95% confidence intervals not crossing over 1.
Bleeding complications, sepsis, and surgical site infection
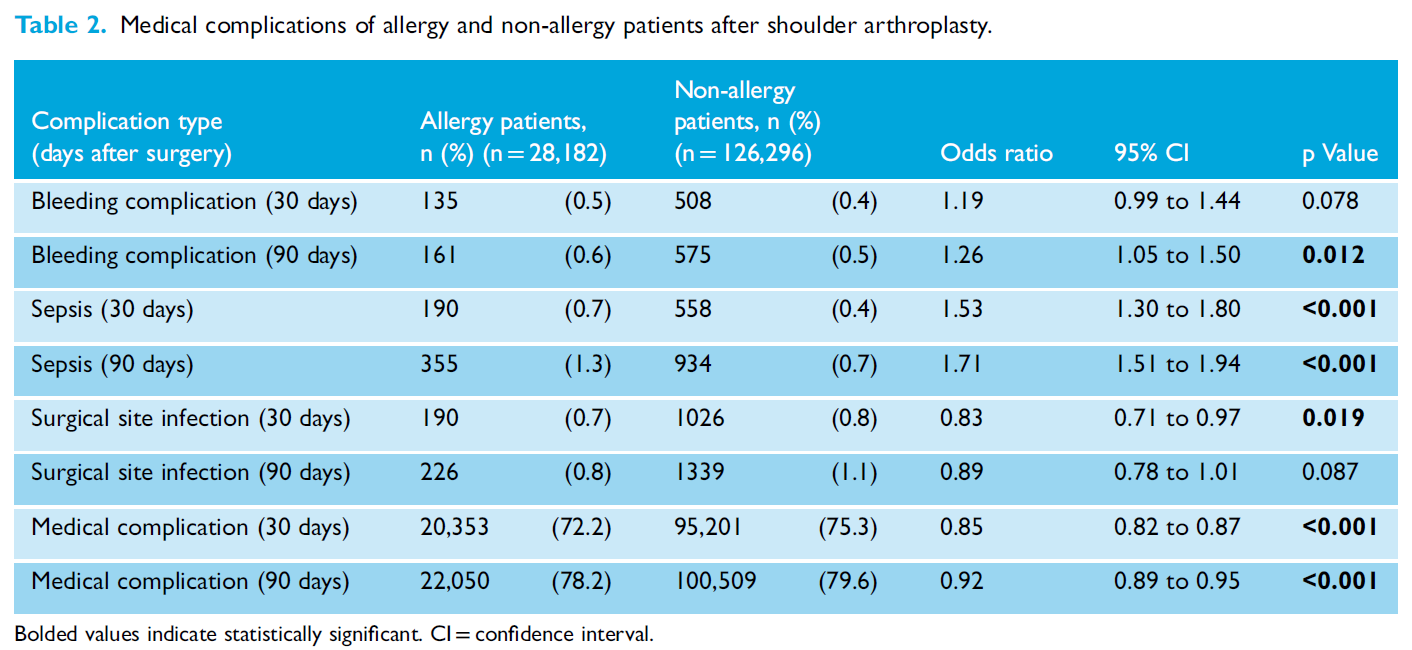
Before we get into ‘medical complications’, I would like to touch on these final three complications. At both time points, sepsis was more associated with patients with an allergy.
An association of bleeding complication and patients with allergies was clinically significant with an OR >1 with the 95% CI above 1. This was at the 90-day time point only. On the other hand, surgical site infection seemed to be less associated with patients with an allergy. This was clinically significant with a OR < 1 with 95% CI below one but this was at the 30-day time point only.
Medical complication
This last complication (shown in the bottom of the table above) confuses me. In the paper, the authors refer to ‘medical complications’ as including bleeding, sepsis, and surgical site infections. This last section suggests that those patients with an allergy have a statistically significant finding of less medical complications than those without an allergy. The OR for both time points are < 1 and the confidence intervals do not go above, or cross 1 suggesting we can have some confidence in these findings.
Why am I be sceptical on this data? We have seen throughout the results in the three tables a fairly consistent finding of complications associated with patients with an allergy. When we look at the total number of patients who were reported to have had a ‘medical complication’, they are huge. For example, at 90 days, 22,050 out of 28,181 patients with an allergy had a ‘medical complication’. This represents 78.2% of the patients. This seems to be a ridiculous proportion of patients given complications rates in the other literature sits around 4-11% for this operation (Craig et al., 2019; Huddleston et al., 2021; Parada et al., 2021). I have sent an email to the authors to clarify this finding. I’ll put an update on here in the near future if I get a response.
Limitations and questions?
With this study being a retrospective analysis on a database, we need to mindful of the validity of the findings. We have to trust individuals that have inputted the complication codes without the rigorous oversight that we would see in a more controlled trial. Without further sub analysis on the type of allergy, we also can’t speculate if one allergy (e.g. metal) is more likely to have worse outcomes than another (e.g. nuts).
Whilst being mindful of the validity of the “medical complication” category, this study paints a picture of a negative outcome in patients with allergies. A hot topic in musculoskeletal practice is around this idea of the negative influence of a low grade inflammatory response that impairs bodily functions and health (Lewis and Fernández-de-las-Peñas, 2022). This may be through medical conditions such as thyroid pathology to smoking or lifestyle related diseases such as diabetes. Could allergies be on this continum?
As always, if anyone has any comments, further reading or suggestions on this topic please feel free to fire them at me on here or on my Twitter. I am always learning and any discrepancies on what I have written is thoroughly encouraged.